ADULT GROWTH HORMONE DEFICIENCY
Description of the Adult GH Deficiency Syndrome
THERE ARE THREE COMPONENTS TO ADULT GH DEFICIENCY
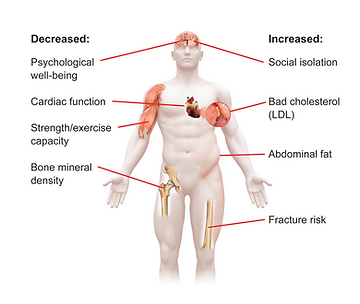
There are three components to the adult GH deficiency syndrome. These are body composition changes, blood lipid (cholesterol and fat) changes, and psychological changes. Because GH maintains muscle and fat, loss of this hormone results in a decrease in muscle and in an accumulation of fat.
The decrease in muscle translates to poor muscle function and decreased exercise capacity. The increase in fat occurs under the skin but also in the abdomen or, more specifically, inside the abdomen. This location is referred to as visceral fat. Medical science has discovered that visceral fat accumulation is especially dangerous because it is associated with an increase in the aging of blood vessels, referred to as atherosclerosis. The blood lipid changes reflect the changes in the fat deposit, and they are all going in the wrong direction. More specifically, there is an increase in the "bad" cholesterol ("LDL cholesterol") and a decrease in the "good" cholesterol ("HDL cholesterol"). There is also an increase in blood triglycerides, another circulating fat, which is associated with blood vessel aging.
The psychological changes associated with GH deficiency have been extensively studied. Patients who develop GH deficiency seem to lose energy. Loss of energy is often the guiding symptom that prompts further investigation. Many individuals with pituitary disease, especially those with other hormone deficiencies, realize that something is missing. Frequently, it turns out to be a deficiency of GH. Individuals with this problem, or their spouses, also notice a loss of interest in their usual hobbies or activities. A decrease in sociability, referred to as social isolation, is another symptom. Patients suffering from this symptom do not like to go out and meet with their friends or social acquaintances. Patients may also develop mild depression or a decrease in sexual function.
Diagnosis of the Adult Growth Hormone Deficiency Syndrome
THERE ARE THREE COMPONENTS TO ADULT GH DEFICIENCY
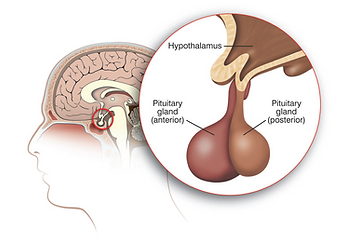
GH deficiency in adults occurs because of some type of injury to the pituitary gland. Injury usually can occur because of the presence of a pituitary tumor, pituitary surgery, or pituitary irradiation. It can also be caused by trauma to the gland or, very rarely, inflammation.
The cause is usually quite obvious to the endocrinologist physician, who will consider the diagnosis of GH deficiency in patients with known pituitary damage. Although GH circulates in the blood, it disappears rapidly from the bloodstream and enters the tissues. Because of this, GH is commonly undetectable in normal individuals as well as in GH-deficient patients. A blood GH level taken randomly, in other words, is usually low. For this reason, endocrinologists need to find another way to prove deficiency of this hormone. This is done by checking to see if stimulating the pituitary releases GH. There are various ways to stimulate the pituitary to release GH (called "GH stimulation tests"). If your physician thinks you may be GH deficient, he or she will usually pick one of the standard tests. The testing is done in the outpatient setting and usually takes about two to three hours. You may be instructed not to eat prior to the test. This type of stimulation testing is necessary not only for medical diagnosis but often for insurance purposes.

Treatment With Growth Hormone
THERE ARE THREE COMPONENTS TO ADULT GH DEFICIENCY
Once a physician has proven GH deficiency, he or she will begin the patient on a small dose of GH and slowly raise the dose until a final maintenance dose is reached. The hormone is given daily by injection. The hormone is given by the patient or a member of the family. Small needles and syringes are used.
The physician will see the patient at four to eight-week intervals to ask how the patient is doing and to obtain a blood test, which can help determine the correct dose. This test is the insulin-like growth factor test ("IGF-1 test"). It is a single blood test that reflects the amount of GH administered, although it is not GH itself. IGF-1 values that are low prompt a larger dose or growth hormone is needed; values that are too high prompt a lower dose. Once a final dose is established, the blood test and office visits will continue approximately every 4 to 6 months. The symptoms of GH excess include muscle or joint pain, retention of fluid (called edema), and carpal tunnel, which consists of pain and/or numbness in the hands. These symptoms, if severe, will also help determine the dose.
There are other ways the physician will monitor GH therapy. If the patient has a pituitary tumor, an MRI will be performed before therapy begins and usually every year thereafter. It is not known whether or not GH can stimulate the growth of residual tumors. The endocrinologist physician will decide when and how often this should be performed. The physician will often elect to monitor blood cholesterol and bone density. Successful therapy is associated with an increase in the density of bones and an improvement in blood cholesterol profile.

Summary
THERE ARE THREE COMPONENTS TO ADULT GH DEFICIENCY
GH deficiency in adults has recently been described. It has recently been approved as an acceptable therapy by the FDA. Most insurance will cover the cost of this medication, which is quite expensive. Improvement in most of the symptoms and body composition changes induced by this deficiency change for the better with successful therapy. GH replacement therapy for GH-deficient adults is considered lifelong therapy.